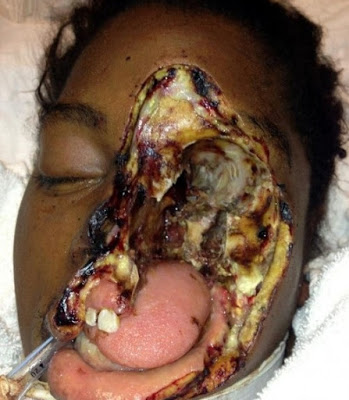
Skin Infection
Skin infection can be caused by a variety of pathogens like bacteria, fungus, parasites and virus. Bacterial infection includes conditions like carbuncle, furuncle, cellulitis, erysipelas, impetigo, ecthyma, necrotizing fasciitis and folliculitis.
Fungal infections include dermatophytosis ringworm (tinea) infection andtinea versicolor. Parasite infections include scabies, pediculosis (lice) and cutaneous larva. Viral infections include Herpes simplex infection, herpes zoster, eczema herpeticum and genital warts. We will discuss them one by one in details below:
Bacterial skin infections
Infections can be caused by bacteria like Staphylococci, Streptococci, Corynebacterium, Propionibacterium, Pseudomonas species & others.
Furuncle
Furuncle is also known as boil resulting from deep seated infection from hair follicle more commonly found on the neck, armpit and groin regions. They appear as red painful lumps which contain pus, like small abscesses.
Skin infection can be caused by a variety of pathogens like bacteria, fungus, parasites and virus. Bacterial infection includes conditions like carbuncle, furuncle, cellulitis, erysipelas, impetigo, ecthyma, necrotizing fasciitis and folliculitis.
Fungal infections include dermatophytosis ringworm (tinea) infection andtinea versicolor. Parasite infections include scabies, pediculosis (lice) and cutaneous larva. Viral infections include Herpes simplex infection, herpes zoster, eczema herpeticum and genital warts. We will discuss them one by one in details below:
Bacterial skin infections
Infections can be caused by bacteria like Staphylococci, Streptococci, Corynebacterium, Propionibacterium, Pseudomonas species & others.
Furuncle
Furuncle is also known as boil resulting from deep seated infection from hair follicle more commonly found on the neck, armpit and groin regions. They appear as red painful lumps which contain pus, like small abscesses.
Furuncle is usually caused by the bacteria Staphylococcus aureus. Predisposing factors include people who are carriers of the bacteria staphylococcus aureus, people with diabetes, excessive sweating, immune deficiency, anemia especially those iron deficient.
Carbuncle
Carbuncle is an aggregation of infected furuncles. Carbuncles may form large abscesses.
General treatment of furuncles and carbuncles include good hygiene, wear loose clothing, use clean linen and cleaning of the infected areas with antiseptic lotion. Target treatment includes oral antibiotics like penicillin and cephalosporin groups. Deeper and serious infection may require intravenous injectable form of antibiotics. For large lesions, surgical intervention incision and drainage may be required.
Carbuncle is an aggregation of infected furuncles. Carbuncles may form large abscesses.
General treatment of furuncles and carbuncles include good hygiene, wear loose clothing, use clean linen and cleaning of the infected areas with antiseptic lotion. Target treatment includes oral antibiotics like penicillin and cephalosporin groups. Deeper and serious infection may require intravenous injectable form of antibiotics. For large lesions, surgical intervention incision and drainage may be required.
Folliculitis
Folliculitis is a skin condition whereby the hair follicles are inflamed and infected. They form tender red spots with pustules filled with pus. It can be superficial or deep infection of the hair follicles involved
Folliculitis is a skin condition whereby the hair follicles are inflamed and infected. They form tender red spots with pustules filled with pus. It can be superficial or deep infection of the hair follicles involved
It can be caused by infection, irritation, hair follicle trauma and occlusion. The commonest pathogen causing folliculitis is Staphylococcus aureus. Predisposing factors include usage of topical steroids, diabetes, immunosuppression, obesity, very frequent shaving, tight clothing and hot humid temperatures.
Treatment generally involves cleansing the affected areas with topical antiseptic solution, avoid tight clothing and practice good personal hygiene. Targeted treatment involves taking oral antibiotics like cloxacillin, erythromycin and cephalexin for about 7-10 days.
If there is scalp folliculitis, cetrimide shampoo may be very helpful and prolonged antibiotics like erythromycin 500mg twice daily or PO doxycycline 100mg twice daily for 4-6 weeks will be necessary for persistent folliculitis.
If there is scalp folliculitis, cetrimide shampoo may be very helpful and prolonged antibiotics like erythromycin 500mg twice daily or PO doxycycline 100mg twice daily for 4-6 weeks will be necessary for persistent folliculitis.
Pseudomonal folliculitis is caused by the bacteria Pseudomonas aeruginosa. People contract it usually after the usage of hot tubs, whirlpools, swimming pools & contaminated bath sponges. The rash typically occur about 8-48 hours post-exposure. It usually resolves on its own by 7-10 days and does not require treatment. However in severe cases, patients can take oral ciprofloxacin for 5-7 days.
Cellulitis
Cellulitis is a bacterial skin infection involving the dermis and subcutaneous layer. It often present as a red, painful swollen area and typically occurs on the legs & near sites of trauma or surgical wounds. As the infection spreads, it may result in an expanding red painful indefinite border on the skin. If the infection is severe, patient may feel generalized unwell, fever, chills, enlarged lymph nodes and septic. Abscesses, blistering, skin erosions and ulcers may also be formed.
Cellulitis
Cellulitis is a bacterial skin infection involving the dermis and subcutaneous layer. It often present as a red, painful swollen area and typically occurs on the legs & near sites of trauma or surgical wounds. As the infection spreads, it may result in an expanding red painful indefinite border on the skin. If the infection is severe, patient may feel generalized unwell, fever, chills, enlarged lymph nodes and septic. Abscesses, blistering, skin erosions and ulcers may also be formed.
It is commonly caused by the bacteria Streptococci & staphylococci aureus. Cellulitis typically occur when there is a breach in the skin caused by a fissure, cut, laceration, insect bite, or puncture wound. Predisposing factors include lymphatic drainage obstruction, diabetes, cancer, venous stasis, immunodeficiency, peripheral arterial disease, chronic liver disease and chronic kidney disease.
Uncomplicated cases can be treated with first line oral antibiotics like amoxicillin plus cloxacillin, co-amoxiclav, cephalexin, erythromycin or clarithromycin for 7-10 days. Second line oral antibiotics for patients allergic to the first line antibiotics include ciprofloxacin 250 – 500mg twice daily or clindamycin 150 – 300mg 4 times daily for 7 – 10 days.
In patients with severe cellulitis, treatment involves intravenous antibiotics crystalline penicillin & cloxacillin followed by oral antibiotics. For patients who are allergic to penicillin, intravenous erythromycin (50 mg/kg/day 4 times daily) or ciprofloxacin 100 – 400mg twice daily.
In patients with abscesses, surgical intervention with incision and drainage may be necessary.
In patients with severe cellulitis, treatment involves intravenous antibiotics crystalline penicillin & cloxacillin followed by oral antibiotics. For patients who are allergic to penicillin, intravenous erythromycin (50 mg/kg/day 4 times daily) or ciprofloxacin 100 – 400mg twice daily.
In patients with abscesses, surgical intervention with incision and drainage may be necessary.
Facial cellulitis and periorbital (around the eyes) cellulitis in young kids less than 3 years old is caused by Haemophilus influenza. In older children, Streptococci & Staphylococci are the causative pathogens. Patient always present with localized swelling of the face, around the eyes associated with redness and pain. Patients usually need to be admitted for further investigations and observation. Complications include otitis media, septicemia (spread of infection to rest of body) and also brain infection.
Treatment usually requires intravenous injectable antibiotics like ampicillin/sulbactam (150 mg/kg/day in divided doses) or ceftriaxone (50 – 100mg/kg/day). If patient is allergic to penicillin, patients can be treated with oral antibiotics erythromycin or cotrimoxazole or intravenous injectable erythromycin 30-50 mg/kg/day in divided doses.
Treatment usually requires intravenous injectable antibiotics like ampicillin/sulbactam (150 mg/kg/day in divided doses) or ceftriaxone (50 – 100mg/kg/day). If patient is allergic to penicillin, patients can be treated with oral antibiotics erythromycin or cotrimoxazole or intravenous injectable erythromycin 30-50 mg/kg/day in divided doses.
Necrotizing fasciitis
Necrotizing fasciitis is a very serious advancing inflammatory infection of the soft tissue, fascia down to the muscles and bones resulting in necrosis of the tissue (death of tissue). Hence it is sometimes called the “flesh eating bacteria infection”. It is caused by the group A beta-hemolytic streptococci. Other possible causative bacteria are Bacteroides, Clostridium, Peptostreptococcus, Enterobacteriaceae, and Escherichia coli, Proteus, Pseudomonas and Klebsiella.
Necrotizing fasciitis is a very serious advancing inflammatory infection of the soft tissue, fascia down to the muscles and bones resulting in necrosis of the tissue (death of tissue). Hence it is sometimes called the “flesh eating bacteria infection”. It is caused by the group A beta-hemolytic streptococci. Other possible causative bacteria are Bacteroides, Clostridium, Peptostreptococcus, Enterobacteriaceae, and Escherichia coli, Proteus, Pseudomonas and Klebsiella.
The bacteria will multiply release toxins and enzymes that result in thrombosis (clotting) of the blood vessels. This result is destruction of the soft tissues and fascia forming necrotic dead tissue. The bacteria can enter via a small cut, graze, pinprick, insect/animal bite or a larger wound due to trauma or surgery. Other predisposing factors include diabetics, immunosuppressed patients, obesity, drug abusers, and people with severe chronic illness.
Clinical presentation of necrotizing fasciitis
The infection typically starts off with an area of redness within hours to days. The redness will spread quickly and the skin will then turn dusky purplish in color. Blisters will also form and the tissue starts to die and become necrotic and turns black. The infection will spread deeper from the skin to subcutaneous area down the fascia to the muscle and bone.
Clinical presentation of necrotizing fasciitis
The infection typically starts off with an area of redness within hours to days. The redness will spread quickly and the skin will then turn dusky purplish in color. Blisters will also form and the tissue starts to die and become necrotic and turns black. The infection will spread deeper from the skin to subcutaneous area down the fascia to the muscle and bone.
The patient will turn very ill, febrile and experience pain in the infected site. As the infection spread, patient may get into toxic shock, low blood pressure and change in conscious level.
Investigations for necrotizing fasciitis
Investigations include full blood count, serum chemistry, blood and tissue cultures to identify the pathogen bacteria involved which will aid in decision on type of antibiotics to use in treatment.
Imaging studies like CT and MRI scan may aid physicians to aid in diagnosis and to determine the extension of infection. A team of physicians comprising of surgeon, infectious disease physician, pathologist and microbiologist.
Investigations for necrotizing fasciitis
Investigations include full blood count, serum chemistry, blood and tissue cultures to identify the pathogen bacteria involved which will aid in decision on type of antibiotics to use in treatment.
Imaging studies like CT and MRI scan may aid physicians to aid in diagnosis and to determine the extension of infection. A team of physicians comprising of surgeon, infectious disease physician, pathologist and microbiologist.
Treatment of necrotizing fasciitis
Necrotizing fasciitis is a surgical emergency and the patient must be admitted to the surgical intensive care unit. The necrotic and infected tissue should be surgically removed and debrided immediately. Early surgical intervention to remove dead tissue can be life-saving, minimize tissue loss and reduce the need or amputation and possible death.
Necrotizing fasciitis is a surgical emergency and the patient must be admitted to the surgical intensive care unit. The necrotic and infected tissue should be surgically removed and debrided immediately. Early surgical intervention to remove dead tissue can be life-saving, minimize tissue loss and reduce the need or amputation and possible death.
Medical treatment involves sufficient hydration, nutrition, hyperbaric oxygen and appropriate intravenous antibiotics. Determining the causative bacteria via cultures results will help aid physician to use the correct high dose antibiotics.
High dose antibiotics should be started immediately to cover aerobic gram-positive and gram-negative organisms and anaerobes. 2 to 3 antibiotics are started to cover aerobes (usually gram-negative organisms), then antibiotics ampicillin and gentamicin are useful. For anaerobes, clindamycin or metronidazole antibiotics are useful.
High dose antibiotics should be started immediately to cover aerobic gram-positive and gram-negative organisms and anaerobes. 2 to 3 antibiotics are started to cover aerobes (usually gram-negative organisms), then antibiotics ampicillin and gentamicin are useful. For anaerobes, clindamycin or metronidazole antibiotics are useful.
Skin grafting will be necessary if there is significant tissue loss and some patients require amputation of limbs to prevent death. Up to 25% of patients will die from the disease. Complications such as renal failure and septicaemia (blood poisoning with bacteria) increase the likelihood of death.
Erysipelas
Erysipelas is bacteria skin infection involving the dermis, subcutaneous area and the lymphatic. The margins of the infection is very clearly demarcated, regional lymph node may enlarged and the skin involved feels hot and tender, often accompanied by fever. The main causative bacteria is mostly Streptococci. Predisposing factors causing erysipelas include trauma, venous & lymphatic insufficiency & sites of superficial fungal infections. Common infectious sites are facial and limbs area.
Erysipelas is bacteria skin infection involving the dermis, subcutaneous area and the lymphatic. The margins of the infection is very clearly demarcated, regional lymph node may enlarged and the skin involved feels hot and tender, often accompanied by fever. The main causative bacteria is mostly Streptococci. Predisposing factors causing erysipelas include trauma, venous & lymphatic insufficiency & sites of superficial fungal infections. Common infectious sites are facial and limbs area.
Usually investigations are not required as treatment is by just antibiotics. Basic investigations like full blood count, ESR, CRP and blood cultures may be required for patients with serious infections. X-ray of sinus may be required for those with facial infection.
Treatment includes penicillin group medications like cephalexin, amoxicillin plus cloxacillin or erythromycin. Alternatives include clarithromycin 250 – 500mg twice daily or co-amoxiclav 625mg twice daily for 7 days or 1gram twice daily for 7 days (in more severe cases). Oral Cotrimoxazole, ciprofloxacin can be used as second line alternatives for patients who are allergic to penicillin.
Treatment includes penicillin group medications like cephalexin, amoxicillin plus cloxacillin or erythromycin. Alternatives include clarithromycin 250 – 500mg twice daily or co-amoxiclav 625mg twice daily for 7 days or 1gram twice daily for 7 days (in more severe cases). Oral Cotrimoxazole, ciprofloxacin can be used as second line alternatives for patients who are allergic to penicillin.
Impetigo
Impetigo is an acute contagious bacteria skin infection caused by Streptococcus pyogenes and/or Staphylococcus aureus bacteria. It is more common in children.
It can be bullous form which consist of blisters which may break and form skin erosions. It can also be in non-bullous form which consists of moist red base filled with yellow crusts. The lesions can be localized or widespread.
Impetigo is an acute contagious bacteria skin infection caused by Streptococcus pyogenes and/or Staphylococcus aureus bacteria. It is more common in children.
It can be bullous form which consist of blisters which may break and form skin erosions. It can also be in non-bullous form which consists of moist red base filled with yellow crusts. The lesions can be localized or widespread.
Impetigo can be caused by contact with a person with impetigo or after skin injury like bites, cuts, abrasions, trauma or infected eczema.
Diagnosis is made by typical history and clinical presentation. Mild impetigo can be treated with topical antibiotic cream like Fusidic acid 2% or mupirocin which can be applied 3 times daily for 5 – 10 days.
Diagnosis is made by typical history and clinical presentation. Mild impetigo can be treated with topical antibiotic cream like Fusidic acid 2% or mupirocin which can be applied 3 times daily for 5 – 10 days.
For more serious infection, it can be treated with oral antibiotics like cloxacillin, cephalexin or co-amoxiclav (Augmentin). Erythromycin can be used for patients who are allergic to penicillin. The localized lesions should be cleansed with antiseptic lotion and crusts should be removed.
For patients with recurrent impetigo, testing if patients are carriers of staphylococcus aureus may be necessary. Infected patients should be abstained from school till recovered.
Ecthyma
Ecthyma is a deeper form of impetigo that extends into the dermis forming covered by adherent crusts. It is caused by the bacteria Streptococcus pyogenes, S. aureus or a combination of the two.
Predisposing risk factors include poor hygiene in a crowded living environment, tropical places with high temperatures and humidity, minor skin injuries, untreated impetigo and immune-compromised patients.
Ecthyma
Ecthyma is a deeper form of impetigo that extends into the dermis forming covered by adherent crusts. It is caused by the bacteria Streptococcus pyogenes, S. aureus or a combination of the two.
Predisposing risk factors include poor hygiene in a crowded living environment, tropical places with high temperatures and humidity, minor skin injuries, untreated impetigo and immune-compromised patients.
Ecthyma lesion often begins as a vesicle (fluid filled bump) over an inflamed skin area which is red and tender. It is often covered with crust. The crust is harder and thicker than that of impetigo. Underneath the crust is red indurated ulcer which oozes pus. It often heals with scarring. Commonly affected sites are buttocks, thighs, legs, ankle and feet. Sometimes local lymph nodes can become swollen and painful.
General measures include proper hygiene and cleaning the affected areas with antiseptic lotion. Topical antibiotics like Fusidic and mupirocin cream can also be used. Oral antibiotics treatment include cloxacillin, cephalexin or erythromycin for 10 to 14 days.
Fungal infection
There are 3 main groups of fungal organisms that can cause skin infections. They include dermatophytes, yeast and moulds. Dermatophytes consist of Tinea corporis, pedis, cruris, capitis, barbae, manuum and Onychomycosis depending on the sites involved. Dermatophytes infection is also called Tinea (fungal infection) which will be discussed in anotherpage on this website.
Yeasts infection consist of candida infection and Malassezia infection likepityriasis versicolor (also known as tinea versicolor). Candida infection also known as candidiasis will be discussed in greater details at an affiliatewebpage. Pityriasis Versicolor is discussed in great detail at another pagein this website.
There are 3 main groups of fungal organisms that can cause skin infections. They include dermatophytes, yeast and moulds. Dermatophytes consist of Tinea corporis, pedis, cruris, capitis, barbae, manuum and Onychomycosis depending on the sites involved. Dermatophytes infection is also called Tinea (fungal infection) which will be discussed in anotherpage on this website.
Yeasts infection consist of candida infection and Malassezia infection likepityriasis versicolor (also known as tinea versicolor). Candida infection also known as candidiasis will be discussed in greater details at an affiliatewebpage. Pityriasis Versicolor is discussed in great detail at another pagein this website.
Parasite skin infections
Parasite infections include scabies, pediculosis (lice) and cutaneous larva.Scabies and lice will be discussed in details at another page in this website.
Cutaneous Larva Migrans
Cutaneous Larva Migrans is a parasite infection caused by hookworm larvae that penetrate the skin and cause red linear itchy rash. It happens more commonly in tropical and subtropical areas. People who go barefoot along beaches, gardeners contact with soil, farmers and pest terminators may be more susceptible.
Parasite infections include scabies, pediculosis (lice) and cutaneous larva.Scabies and lice will be discussed in details at another page in this website.
Cutaneous Larva Migrans
Cutaneous Larva Migrans is a parasite infection caused by hookworm larvae that penetrate the skin and cause red linear itchy rash. It happens more commonly in tropical and subtropical areas. People who go barefoot along beaches, gardeners contact with soil, farmers and pest terminators may be more susceptible.
The parasites eggs are passed from animal feces into the soil where they hatch into larva. They penetrate the skin of animal hosts and is carried by the venous and lymphatics system to the lungs and subsequently to the trachea whereby they will be swallowed and finally reach the intestines. In the intestine the mature and then get passed out in the feces again. Human happen to be the accidental host and the larva remains in the skin until they die off they do not migrate to the intestines.
Cutaneous Larva Migrans is a benign, self-limiting condition that can affect any ages. Clinical presentation includes prickling or tingling sensation within 30 minutes of larva penetration. The larvae may remain dormant for weeks or they may creep and form red snake-like tracks (consisting of papules/vesicles) from site of penetration. These tortuous tracks may advance 1 to 2 cm daily and cause extreme itch. Common sites involve are the feet, hands, knees and buttocks. The larva will eventually die.
Diagnosis is clinical and laboratory tests are not required. As it is a self-limiting condition which will recover in 4-8 weeks, treatment may not be required. Antihistamines can be given to ease the itch. Anti-parasites agent like topical thiabendazole cream can be applied on localized lesion. Other effective alternative medications include albendazole, mebendazole, and ivermectin. Oral medications should be considered if topical treatment fails or if the area involved is generalized. Itch tend to reduce within 1-2 days and the tracks of larvae should remiss within a week.
If there is secondary skin infection, antibiotics can be given for treatment. Liquid nitrogen can also be used to try to freeze the end of the larva burrow.
Viral Skin Infections
Viral skin infections consist of herpes virus infection which can cause herpes type 1 & type 2 herpes which affects genitalia area and also herpes zoster infection (shingles). Eczema Herpeticum refers to herpes skin infection on patients who have eczema. HPV virus infection can cause warts and often genital warts which is sexually transmitted which will be discussed at another webpage.
Type 1 Herpes Simplex Virus
Type 1 Herpes Simplex Virus (HSV) infection is often called cold sores which presents as vesicles and blisters around the lips and facial area (Herpetic Gingivostomatitis). 80% of HSV infection does not cause any symptoms and the virus just lie latent resting state in the nerves. HSV does not cause mortality unless it infects fetus during pregnancy, encephalitis (brain infection) and other serious infection in the immune-compromised.
Viral skin infections consist of herpes virus infection which can cause herpes type 1 & type 2 herpes which affects genitalia area and also herpes zoster infection (shingles). Eczema Herpeticum refers to herpes skin infection on patients who have eczema. HPV virus infection can cause warts and often genital warts which is sexually transmitted which will be discussed at another webpage.
Type 1 Herpes Simplex Virus
Type 1 Herpes Simplex Virus (HSV) infection is often called cold sores which presents as vesicles and blisters around the lips and facial area (Herpetic Gingivostomatitis). 80% of HSV infection does not cause any symptoms and the virus just lie latent resting state in the nerves. HSV does not cause mortality unless it infects fetus during pregnancy, encephalitis (brain infection) and other serious infection in the immune-compromised.
Causes: Type 1 HSV infection is usually transmitted by direct contact with infected secretions like saliva & genital secretions. Unlike Type 2 HSV infection it is less likely through sexual contact unless patient engage in oral sex. Minor trauma like cuts and abrasions can also cause the virus to inoculate into the skin. After acquiring HSV, the virus will remain dormant in the nerves, replicate and reactivate to cause symptoms. Factors resulting in reactivation will be fever, infections, trauma, emotional stress, sunlight exposure and menstruation.
Clinical presentation: Type 1 HSV infection also known as Gingivostomatitis can be contracted by infected saliva. The incubation period is about 3 to 6 days. It typically affect young children from 6 months to 5 years old. It can also affect adults.
There will be an abrupt onset of fever, lethargy, red swollen gums, vesicles (fluid filled small bumps) on the tongue, lips and around the mouth, ulcers and sometimes enlarged neck lymph nodes. It may last about 1-2 weeks. Infected person may pass on to another person via infected saliva for up to 3 weeks. In adults they may experience pharyngitis (infected pharynx) and tonsillitis (infected tonsil) causing extreme sore throat and painful swallowing.
There will be an abrupt onset of fever, lethargy, red swollen gums, vesicles (fluid filled small bumps) on the tongue, lips and around the mouth, ulcers and sometimes enlarged neck lymph nodes. It may last about 1-2 weeks. Infected person may pass on to another person via infected saliva for up to 3 weeks. In adults they may experience pharyngitis (infected pharynx) and tonsillitis (infected tonsil) causing extreme sore throat and painful swallowing.
Patients may have recurring HSV infection which may be triggered by trauma, emotional stress, infection and hormonal changes during menstruation.
Complications: Lesions around the eye can cause eye infection and corneal ulcer, eczema Herpeticum (severe rash in patients with eczemaassociated with blisters, scabs, swollen lymph nodes and fever), nerves in face may be infected causing temporarily muscle paralysis and widespread infection in immune-suppressed patients.
Complications: Lesions around the eye can cause eye infection and corneal ulcer, eczema Herpeticum (severe rash in patients with eczemaassociated with blisters, scabs, swollen lymph nodes and fever), nerves in face may be infected causing temporarily muscle paralysis and widespread infection in immune-suppressed patients.
Diagnosis: is usually by its typical clinical picture and laboratory tests to isolate the herpes simplex virus. HSV can be isolated from the lesions via Tzank smears, detection of HSV DNA via PCR or Direct fluorescent antigen (DFA can distinguish different herpes viruses and non-herpes viruses). HSV antibody testing for type 1 and type 2 herpes simplex virus can be done to test if patient has been infected with the virus before.
Treatment: Very mild uncomplicated cold sores do not usually require treatment. Antiviral drugs can be used to reduce the virus from multiplying to shorten the clinical course however it does not eradicate the dormant virus in the nerve cells. Recurrent attacks may be prevented by taking continuous dose of medications.
Topical antiviral cream like aciclovir may shorten the clinical course of mild disease. Oral antiviral tablets may be necessary for more severe condition. Doses include aciclovir 200mg five times daily for 5 days or valaciclovir 1 gram three times daily for 7 days or famciclovir as a single dose of 3 x 500mg.
Topical antiviral cream like aciclovir may shorten the clinical course of mild disease. Oral antiviral tablets may be necessary for more severe condition. Doses include aciclovir 200mg five times daily for 5 days or valaciclovir 1 gram three times daily for 7 days or famciclovir as a single dose of 3 x 500mg.
Type 2 Herpes simplex virus
Type 2 HSV infection is a sexually transmitted disease resulting in genital ulcers and lesions. The clinical course and treatment plan will be discussed on another webpage.
Type 2 HSV infection is a sexually transmitted disease resulting in genital ulcers and lesions. The clinical course and treatment plan will be discussed on another webpage.
Herpes Zoster (Shingles)
Herpes zoster (Varicella Zoster) also known as shingles is caused by reactivation of previous chickenpox virus that has lie dormant in the nerve cells. The incidence of shingles increases with age, more than 66% of patients are older than 50 years old. It is rare in children and young adult unless their immune system is compromised.
Triggers for the reactivation of the dormant varicella-zoster virus include external re-exposure to the virus, acute infection, chronic diseases that weaken the immune system, emotional stress and certain immunosuppressive drugs.
Herpes zoster (Varicella Zoster) also known as shingles is caused by reactivation of previous chickenpox virus that has lie dormant in the nerve cells. The incidence of shingles increases with age, more than 66% of patients are older than 50 years old. It is rare in children and young adult unless their immune system is compromised.
Triggers for the reactivation of the dormant varicella-zoster virus include external re-exposure to the virus, acute infection, chronic diseases that weaken the immune system, emotional stress and certain immunosuppressive drugs.
Clinical presentation: Initially patient will start with a prodromal symptoms like fever, lethargy and lack of appetite. Patient will have severe pain in the sensory root. After the pain starts 1-3 days later, patient will experience a blistering vesicular (group of fluid filled bumps) rash with pustules over the painful site following a nerve root forming a belt. The regional lymph nodes may also be enlarged and inflamed. The lesions commonly occur on the forehead near the eye (ophthalmic region), chest, neck and lower back areas. Patients will recover in 2-3 weeks for uncomplicated cases and in about 4-6 weeks in older patients.
Herpes zoster ophthalmicus: When cranial nerve 5 (trigeminal nerve) is infected by the virus, it causes lesions around the eye. Eye may be affected causing inflammation of the conjunctiva, sclera, corneal ulcer, sometimes paralysis of eye muscles, and glaucoma and vision disturbance due to optic nerve involvement. An ophthalmologist consult is warranted to look for early signs of visual disturbances.
Ramsay Hunt Syndrome: The zoster vesicles will occur around the external ear/ tympanic membrane, causing ear pain, facial nerve palsy (resulting in asymmetry of face with one sided droopy mouth), reduced hearing and sometimes vertiginous giddiness.
Serious complications occur in those who has suppressed immune system. The complications include encephalitis (infection of brain), disseminated shingles (generalized body rash is involved), visceral involvement (spread of infection to other organs), pneumonia, chronic fatigue syndrome, muscle weakness and post herpetic neuralgia.
Post-herpetic Neuralgia: refers to the persistent or recurrent feeling of pain or numbness along the nerve root even after infection. It can be controlled with pain relief.
Diagnosis: is made by shingles typical clinical history and signs. Laboratory test is rarely necessary.
Treatment: General measures include avoid contact of lesions with uninfected person. In uncomplicated cases in healthy people, shingles usually is self-limiting and no treatment is required. However if there is pain or more severe infection, anti-viral medication can reduce the symptoms and duration of the course of the zoster infection. Immune-compromised and patients with very severe complications require hospitalization and also intravenous antiviral medications. If there is secondary bacteria infection of the skin, antibiotics will be prescribed.
Normal saline or calamine lotion can be applied onto the skin lesions. Oral anti-viral drugs like aciclovir 800 mg 5 times daily, valaciclovir 1 gram 3 times daily and famciclovir 500 mg 3 times daily for 7-10 days can be prescribed to hasten recovery and reduce symptoms. Treatment is most effective if started within 72 hours of disease eruption.
Treatment: General measures include avoid contact of lesions with uninfected person. In uncomplicated cases in healthy people, shingles usually is self-limiting and no treatment is required. However if there is pain or more severe infection, anti-viral medication can reduce the symptoms and duration of the course of the zoster infection. Immune-compromised and patients with very severe complications require hospitalization and also intravenous antiviral medications. If there is secondary bacteria infection of the skin, antibiotics will be prescribed.
Normal saline or calamine lotion can be applied onto the skin lesions. Oral anti-viral drugs like aciclovir 800 mg 5 times daily, valaciclovir 1 gram 3 times daily and famciclovir 500 mg 3 times daily for 7-10 days can be prescribed to hasten recovery and reduce symptoms. Treatment is most effective if started within 72 hours of disease eruption.
Pain killers like paracetamol, NSAIDs, narcotics (tramadol and codeine), anti-depressants like (TCA), anticonvulsant drugs (carbamazepine and gabapentin), topical creams that contain capsaicin or lidocaine, Botox injections and Transcutaneous Electrical Nerve stimulation can be used to control post-herpetic neuralgia. In some cases, physicians prescribe steroid to reduce inflammation of nerve roots.
Prevention of herpes zoster: Varicella-Zoster vaccine (Zostavax) has been available to prevent shingles. The vaccine is 14 times more potent than chickenpox vaccine. It is a live vaccine hence it cannot be used on patients whose immune system is compromised. The vaccine has been found to reduce occurrence by 50% in patients older than 60 years, by 64% in those aged 60-69 years, and by 70% in subjects aged 50-59 years. It also reduces pain compared with those without vaccination before. A single dose of Zostavax given subcutaneously is recommended for those above 50 years old.
For those who have been exposed to shingles via close contact with infected person, Varicella- Zoster Immune globulin injection may be injected to prevent the development of full blown shingles. It should be administered within 96 hours and allow protection up to 3 weeks.
Eczema Herpeticum
Eczema Herpeticum is a complication of patients who has an eczema flare and co-existing herpes simplex virus. It was previously known as Kaposi varicelliform eruption as it resembles chickenpox. It is more common in infants and young children with underlying eczema condition.
Eczema Herpeticum is a complication of patients who has an eczema flare and co-existing herpes simplex virus. It was previously known as Kaposi varicelliform eruption as it resembles chickenpox. It is more common in infants and young children with underlying eczema condition.
Certain conditions that cause breakdown of skin barrier can also precipitate eczema Herpeticum. The conditions include ichthyosis, cutaneous T cell lymphoma, mycosis fungoides, darier disease, thermal burn injuries, pemphigus vulgaris and viruses like coxsackievirus A16.
Clinical presentation: Patient will be unwell, having fever and sudden onset of clusters of itchy painful blisters. New lesions will occur and spread over a period of 7-10 days. The blisters may be filled with yellow purulent fluid or blood. The blisters may form crusts, erosions and ulcers. It will take about 2-6 weeks for the lesion to totally heal.
Clinical presentation: Patient will be unwell, having fever and sudden onset of clusters of itchy painful blisters. New lesions will occur and spread over a period of 7-10 days. The blisters may be filled with yellow purulent fluid or blood. The blisters may form crusts, erosions and ulcers. It will take about 2-6 weeks for the lesion to totally heal.
Secondary bacterial infection with streptococcus and staphylococcus will lead to impetigo and cellulitis described above. Post infection, lesions may heal with remnant scars. Very severe infection that has spread throughout the body (disseminated infection) in the immune compromised patients can be very serious.
Diagnosis: can be confirmed by a viral swab from a blister/vesicle that is sent for tests like Direct Fluorescent Antibody (DFA) stain, PCR (Polymerase Chain Reaction) sequencing and Tzank smear (reveal epithelial multinucleated giant cells and acantholysis) to identify the HSV virus.
Bacterial swabs can be taken for bacterial culture to identify any pathogen that could have caused secondary bacterial infections. If diagnosis is in doubt, biopsy of the lesion and histological examination will confirm the diagnosis.
Treatment of eczema Herpeticum: Eczema Herpeticum is a dermatology emergency, early administering anti-viral medication may reduce the need for hospitalization, complications and reduce morbidity.
Antiviral drugs: In adults, oral aciclovir 400 to 800 mg 5 times daily or valaciclovir 1 g twice daily for 10 to 14 days can be given until lesions heal. In children, suspension form of antiviral medications with dosage according to the child's age can be given. Intravenous aciclovir is necessary in severe infection or infection that does not respond to oral tablets.
Treatment of eczema Herpeticum: Eczema Herpeticum is a dermatology emergency, early administering anti-viral medication may reduce the need for hospitalization, complications and reduce morbidity.
Antiviral drugs: In adults, oral aciclovir 400 to 800 mg 5 times daily or valaciclovir 1 g twice daily for 10 to 14 days can be given until lesions heal. In children, suspension form of antiviral medications with dosage according to the child's age can be given. Intravenous aciclovir is necessary in severe infection or infection that does not respond to oral tablets.
Antibiotics like penicillin, cephalosporin and erythromycin are prescribed if there is secondary skin bacterial infection.
Ophthalmologist consult is warranted if there is eye involvement as keratitis may cause scarring and other eye complications include optic neuritis which may affect vision.
Ophthalmologist consult is warranted if there is eye involvement as keratitis may cause scarring and other eye complications include optic neuritis which may affect vision.